Along with all of the daily radiation treatments and in-home nurse visits, my busy schedule had to accommodate regular clinic visits as well. At first they occurred more than once a week, and then after treatment ended the time between visits was increased. It was important that every aspect of my health and other aspects of my well-being were monitored.
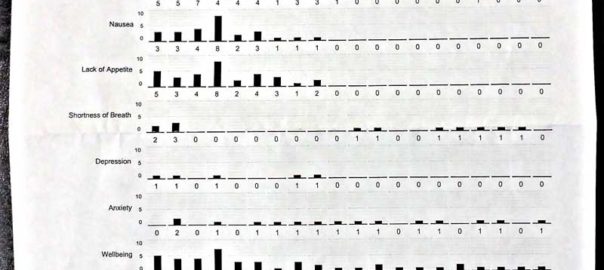
After registering at reception, the weekly clinic visit started off with a wellness quiz. On a scale of 1 to 10 (10 being the worst), I was asked to evaluate every aspect of my well-being: pain, drowsiness, tiredness, lack of appetite, shortness of breath, depression, anxiety, and overall wellbeing. In addition, I was asked to assess how normal my activities and functionality were on a scale of 1 to 5: worst being not able to get out of bed and needing assistance for everything, and best being able to manage all tasks normally. Since the quiz was computerized, it kept track of how I was doing for each of the wellness scales. The quiz shown starts in March of 2014, just about a month after my radiation treatments started and after my first chemo. It was pretty rough during the treatment time period, but it’s not hard to see where the gradual improvement of my health and wellbeing started.

After the wellness quiz, which took longer to print the results than it did to actually complete the quiz, it was off to the lab to get blood work done. I’d go take a number, then sit and wait for my number to come up, only to be told that they couldn’t use my PICC line: only qualified nurses could draw blood from it and the lab technicians weren’t qualified. It wasn’t until several weeks had passed that a technician casually mentioned to me I could go get my blood drawn by a chemo nurse, and I could bypass being poked. Hallelujah!
Once the chemo nurses started drawing the blood for my lab tests, they could kill two birds with one stone. My PICC line needed weekly flushing and the dressing changed, so they would take care of that as well. Since the PICC line was already inserted into a major vein in my arm, there weren’t any further pricks. The only drawback was when they flushed it: I immediately experienced a very metallic taste in my mouth. I’ll just add one word of advice to anyone using a PICC line: you have to keep it dry in the shower. I found that wrapping my arm with “Press ‘n Seal” worked wonders: it stuck to the skin and really created a waterproof barrier.
While we waited for the blood test results, the triage nurse took over. She perused my quiz results to see if there was anything to be overly concerned about, then she weighed me (ugh) and checked my temperature.
After her was the visit with the Chemo Oncologist who reviewed the quiz and blood results. More often than I cared, he found issues with the blood work and faster than you can say “Bob’s your uncle” (which he is 😉 ) I’d be whisked off for another calcium or magnesium infusion. There goes another 6 hours of unscheduled time. After the first time of being caught unprepared for an extended stay, we started packing a day case with meds, feeding solution, cell phone chargers, food for Seaghan, water, etc.
Next up is the Radiation Oncologist. While I was undergoing radiation treatments his clinics were held in the radiation unit area every Wednesday afternoon, and once treatments were done he’d see me in the regular clinic area of the hospital. He’d check my skin, feel my neck, check the feeding tube, and check my throat. He was usually accompanied by the Dietician who made sure that I was able to continue with the feedings as scheduled, and that I was maintaining weight.
Even though I’d seen the Microsurgeon before treatment started, he would not be part of the clinic visits until after I’d finished treatments. More on that later.
—Sandi
Next time: yet even more side effects, on the positive side!
Always a fascinating read. I’m glad that you’re sharing this incredible story with us.